ACLS Tachycardia Algorithm
Emergency Protocol for Fast Heart Rate
Comprehensive ACLS tachycardia algorithm for healthcare professionals managing patients with fast heart rates. Includes assessment criteria, cardioversion protocols, and medication guidelines.
Tachycardia Definition & Recognition
Definition
- • Heart rate typically ≥150/min if tachyarrhythmia
- • Assess appropriateness for clinical condition
- • Consider patient's age, fitness level, and clinical context
- • May be physiologically appropriate in some situations
Signs of Instability
- • Altered mental status
- • Ischemic chest discomfort
- • Acute heart failure
- • Hypotension with signs of shock
- • Syncope
- • Other signs of poor perfusion
Assessment and Initial Management
Step-by-Step Assessment
- 1Assess appropriateness for clinical condition
Heart rate typically ≥150/min if tachyarrhythmia
- 2Identify and treat underlying causes
Look for reversible causes and contributing factors
- 3Maintain patent airway; assist breathing as necessary
Ensure adequate oxygenation and ventilation
- 4Give oxygen if hypoxemic
Target SpO2 ≥94% unless contraindicated
- 5Monitor blood pressure and oximetry
Continuous monitoring of vital signs
- 6Establish IV access
Prepare for medication administration
- 712-Lead ECG if available; don't delay therapy
Identify rhythm and QRS width
Treatment Decision Tree
Does patient have signs of poor perfusion?
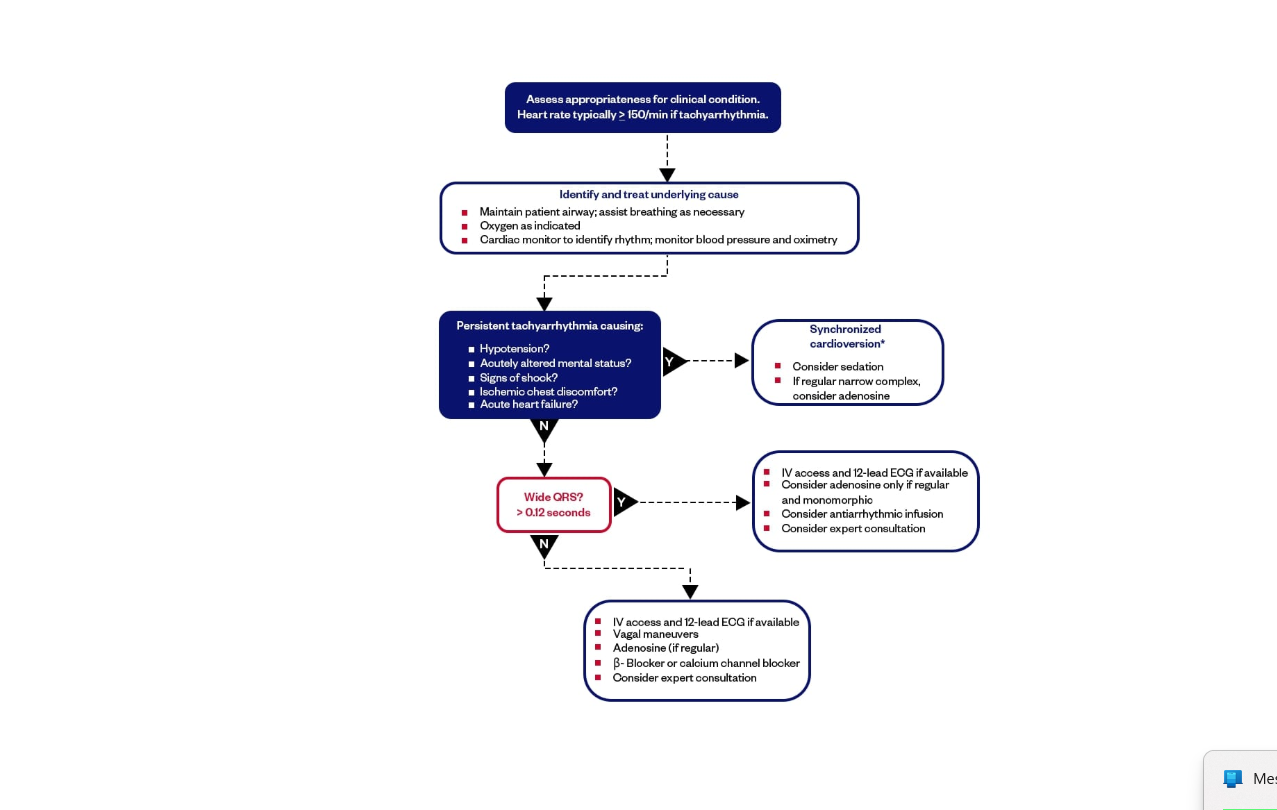
YES - Symptomatic Tachycardia
Immediate synchronized cardioversion
- • Consider sedation if time permits
- • Synchronized cardioversion
- • If unsuccessful, increase energy
NO - Stable Tachycardia
Wide QRS (≥0.12 sec):
- • CPR 2 minutes
- • Adenosine (if regular)
- • Antiarrhythmic infusion
- • Expert consultation
Narrow QRS:
- • High-quality CPR is critical
- • Vagal maneuvers
- • Adenosine
- • β-Blocker or calcium channel blocker
Medication Protocols
Adenosine
Dosing:
- • First dose: 6 mg rapid IV push
- • Second dose: 12 mg if first dose ineffective
- • Follow each dose with 20 mL normal saline flush
- • Give through most proximal IV site
Mechanism:
Blocks AV node conduction temporarily
Contraindications:
- • Irregular rhythms
- • Second or third-degree AV block
- • Known accessory pathway (WPW)
Alternative Treatments
β-Blockers:
- • Metoprolol: 2.5-5 mg IV every 2-5 minutes
- • Esmolol: 0.5 mg/kg loading dose
- • Propranolol: 0.1 mg/kg IV divided into 3 doses
Calcium Channel Blockers:
- • Diltiazem: 0.25 mg/kg IV over 2 minutes
- • May repeat with 0.35 mg/kg if needed
- • Maintenance infusion: 5-15 mg/hr
Antiarrhythmics:
- • Amiodarone: 150 mg IV over 10 minutes
- • Procainamide: 20-50 mg/min until suppressed
- • Sotalol: 100 mg IV over 5 minutes
Synchronized Cardioversion
Energy Recommendations
Narrow Regular:
50-100 J
Narrow Irregular:
120-200 J
Wide Regular:
100 J
Wide Irregular:
Defibrillation dose (not synchronized)
Procedure
- 1. Consider sedation if time permits
- 2. Ensure sync mode is activated
- 3. Select appropriate energy level
- 4. Charge and deliver shock
- 5. Check rhythm and pulse
- 6. If unsuccessful, increase energy and repeat
Reversible Causes of Tachycardia
H's (Hypoxia, Hypovolemia, etc.)
- • Hypoxia: Ensure adequate oxygenation
- • Hypovolemia: IV fluid resuscitation
- • Hydrogen ions (acidosis): Correct pH
- • Hyperkalemia/Hypokalemia: Correct electrolytes
- • Hypothermia: Rewarm gradually
- • Hypoglycemia: Give glucose if indicated
T's (Toxins, Tamponade, etc.)
- • Toxins: Consider antidotes
- • Tamponade: Pericardiocentesis
- • Tension pneumothorax: Needle decompression
- • Thrombosis (coronary): PCI/thrombolytics
- • Thrombosis (pulmonary): Anticoagulation
- • Trauma: Address underlying injuries
Master ACLS Tachycardia Management
Tachycardia management requires quick assessment and appropriate intervention. Get certified in ACLS to confidently manage these critical situations.
