866.721.1749
services@comrestraining.com
Serving communities nationwideNationwide
ACLS Bradycardia Algorithm
Emergency Protocol for Slow Heart Rate
Comprehensive ACLS bradycardia algorithm for healthcare professionals managing patients with slow heart rates and signs of poor perfusion.
Bradycardia Definition & Recognition
Definition
- • Heart rate <60 beats per minute
- • Inappropriate for clinical condition
- • May be physiologically normal in some patients
- • Consider patient's baseline and clinical context
Signs of Poor Perfusion
- • Altered mental status
- • Chest pain or discomfort
- • Hypotension (SBP <90 mmHg)
- • Signs of shock (cool, clammy skin)
- • Acute heart failure
- • Syncope or near-syncope
Assessment and Initial Management
Step-by-Step Assessment
- 1Assess appropriateness for clinical condition
Consider patient's age, fitness level, medications, and baseline
- 2Identify and treat underlying causes
Look for reversible causes (H's and T's)
- 3Maintain patent airway; assist breathing as necessary
Ensure adequate oxygenation and ventilation
- 4Give oxygen if hypoxemic
Target SpO2 ≥94% unless contraindicated
- 5Monitor blood pressure and oximetry
Continuous monitoring of vital signs
- 6Establish IV access
Prepare for medication administration
- 712-Lead ECG if available
Identify rhythm and look for underlying causes
Treatment Decision Tree
Does patient have signs of poor perfusion?
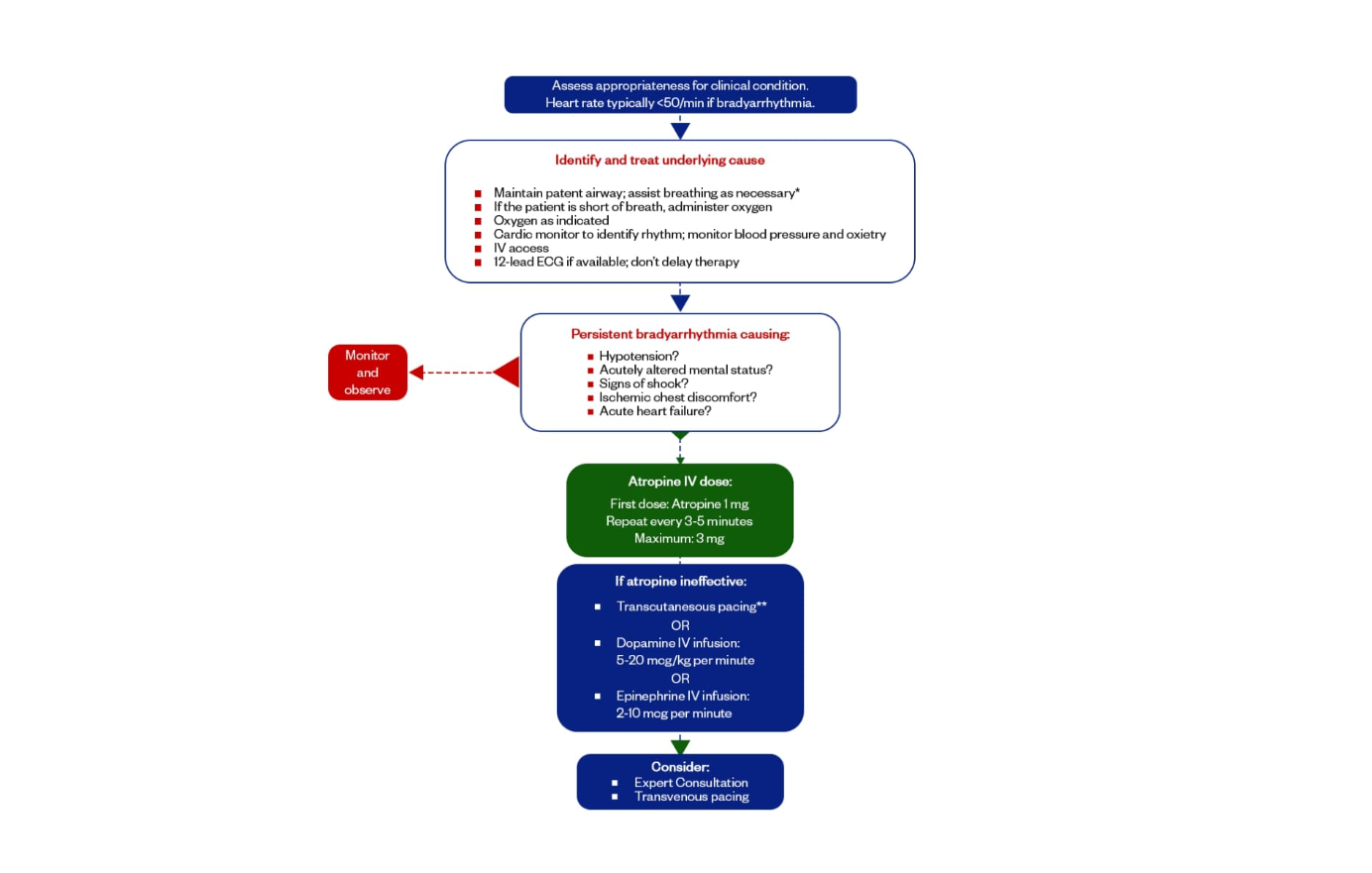
YES - Symptomatic Bradycardia
Immediate Actions:
- 1. Atropine 1 mg IV push
- 2. May repeat every 3-5 minutes
- 3. Maximum total dose: 3 mg
If Atropine Ineffective:
- • Transcutaneous pacing
- • Dopamine 5-20 mcg/kg/min
- • Epinephrine 2-10 mcg/min
- • Consider transvenous pacing
NO - Asymptomatic
Continue Monitoring:
- • Observe for changes
- • Monitor vital signs
- • Identify underlying causes
- • Prepare for intervention if needed
Consider:
- • Expert consultation
- • Cardiology evaluation
- • Medication review
- • Electrolyte correction
Medication Protocols
Atropine
Dosing:
- • First dose: 1 mg IV push
- • Repeat: 1 mg every 3-5 minutes
- • Maximum total: 3 mg
- • Minimum dose: 0.5 mg (avoid paradoxical bradycardia)
Mechanism:
Blocks vagal stimulation, increases SA node firing rate and AV conduction
Contraindications:
- • Hypothermic bradycardia
- • Second or third-degree AV block with wide QRS
- • Transplanted heart
Alternative Treatments
Dopamine Infusion:
- • Dose: 5-20 mcg/kg/min
- • Titrate to adequate perfusion
- • Monitor for arrhythmias
Epinephrine Infusion:
- • Dose: 2-10 mcg/min
- • Alternative to dopamine
- • Titrate to effect
Transcutaneous Pacing:
- • Consider early if atropine unlikely to work
- • Use analgesics/sedation if conscious
- • Verify mechanical capture
Reversible Causes of Bradycardia
H's (Hypoxia, Hypovolemia, etc.)
- • Hypoxia: Ensure adequate oxygenation
- • Hypovolemia: IV fluid resuscitation
- • Hydrogen ions (acidosis): Correct pH
- • Hyperkalemia/Hypokalemia: Correct electrolytes
- • Hypothermia: Rewarm gradually
- • Hypoglycemia: Give glucose if indicated
T's (Toxins, Tamponade, etc.)
- • Toxins: Consider antidotes (digoxin, beta-blockers, calcium channel blockers)
- • Tamponade: Pericardiocentesis if indicated
- • Tension pneumothorax: Needle decompression
- • Thrombosis (coronary): Consider PCI/thrombolytics
- • Thrombosis (pulmonary): Anticoagulation/embolectomy
- • Trauma: Address underlying injuries
Special Considerations
Pediatric Considerations
- • Bradycardia in children is usually due to hypoxia
- • Focus on airway and breathing first
- • CPR if HR <60 with poor perfusion
- • Epinephrine is first-line drug
Drug-Induced Bradycardia
- • Beta-blockers: Consider glucagon
- • Calcium channel blockers: Consider calcium, glucagon
- • Digoxin: Consider digoxin-specific antibodies
- • Clonidine: Supportive care
When to Avoid Atropine
- • Hypothermic patients
- • Heart transplant recipients
- • High-degree AV blocks with wide QRS
- • May worsen ischemia in some cases
Transcutaneous Pacing
Indications
- • Symptomatic bradycardia unresponsive to atropine
- • High-degree AV block
- • Bradycardia with escape rhythms
- • Overdose of calcium channel blockers or beta-blockers
- • Immediately available when atropine is unlikely to be effective
Procedure
- 1. Apply pacing pads (anterior-posterior preferred)
- 2. Set rate to 60-70 bpm
- 3. Set output to 2 mA above threshold
- 4. Verify electrical and mechanical capture
- 5. Provide analgesia/sedation if conscious
- 6. Prepare for transvenous pacing if prolonged
Key Clinical Points
Remember:
- • Not all bradycardia requires treatment
- • Treat the patient, not the monitor
- • Address underlying causes first
- • Consider expert consultation early
Critical Actions:
- • Ensure adequate oxygenation
- • Establish IV access early
- • Monitor for deterioration
- • Prepare for transcutaneous pacing
Master ACLS Bradycardia Management
Bradycardia management requires quick assessment and appropriate intervention. Get certified in ACLS to confidently manage these critical situations.
